Karnataka 2nd PUC Biology Notes Chapter 3 Human Reproduction
Reproduction is the process by which, an organism produces offsprings of its own kind. It ensures the passage of genetic material from generation to generation and maintains the continuity of the species. Thus it is the mechanism by which the thread of life is sustained. The maturity or puberty of male starts from, 20 -21 years to 80 years, but in female it is from 13-15 years upto 50 years.
Male reproductive system:
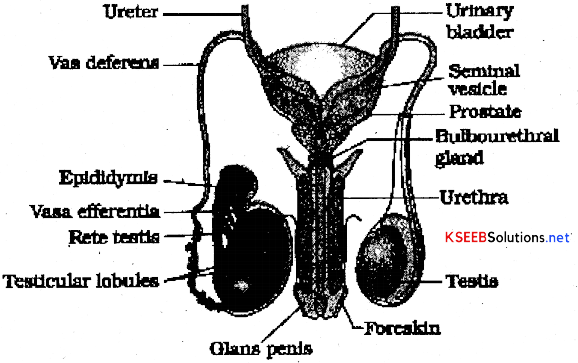
→ Male reproductive system consists of a pair of testes, a pair of epididymis, a pair of vas deferens, a pair of ejaculatory ducts, a penis and accessory glands in the form of seminal vesicles, prostate glands and bulbourethral glands.
→ Testes are found suspended in an outpouching of the skin called the scrotum, present below the pelvic region out side the body. Each testis contains a number minute microscopic tubules called seminiferous tubules. The seminiferous tubules are lined by spermatogonial cells and sertoli cells/ Spermatogonial cells give rise to sperms and sertoli cells provide nursing support to the spermatids and secrete a hormone called inhibin. Groups of interstitial cells or cells of Leydig are present between the seminiferous tubules. They secrete male sex hormones called androgens like testosterone.
![]()
→ Epididymis are paired comma shaped structures. Seminiferous tubules of each testis open into an epididymis through Vas efferentia (small ducts) which carry the sperms into them. Epididymis serves as an organ for storage and transportation of sperms.
→ Each epididymis opens into a sperm duct called vas deferens or ductus deferens which is about 45cm. long. The vas deferens of each side ascends along the testis and runs upwards into the body to open into the ejaculatory duct into which the seminal vesicle opens. Both the ejaculatory ducts open into the upper part of a common tube called the Urethra which opens to the outside through the urethral orifice at the tip of the penis.
→ Penis is an erectile muscular organ used for micturition and to introduce spermatozoa into the vagina during intercourse. Internally the penis is composed of three cylindrical masses of tissues, two dorsolateral and a midventral mass. These tissues are erectile, contain blood sinuses and bound together by fibrous tissue. The enlarged distal end of the penis is called the glans. It is covered by a loose-fitting skin called prepuce or foreskin.
Table showing functions of the male reproductive system:
| Parts of the reproductive system | Functions |
| Testis | Production of sperms and the male sex hormone |
| Epididymis | Storage and maturation of sperms |
| Vas deferens | Transportation of sperms |
| Ejaculatory duct | Conduction of sperms |
| Penis | Organ of sexual intercourse |
| Accessory Glands | Conduction of sperms secretion make up large portion of semen |
| Seminalvesicle | Conduction of sperms secretion make up large portion of semen |
| Prostate gland | Secreations make up large portion of semen and help sperm motility gland |
| Bulbourethral | Secretions provide lubrication and make up a large portion of semen. |
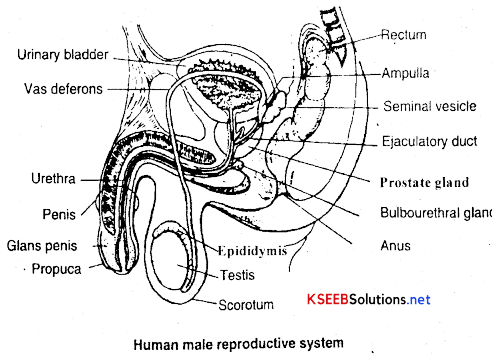
Seminal vesicles are paired convoluted accessory glands. They secrete ah alkaline mucoid secretion containing fructose, ascorbic acid etc., which form a major part of the ejaculated semen.
Prostate is a single accessory gland present below the neck of the urinary bladder. It secretes a thin milky fluid which forms a part of the semen and helps sperm motility.
Bulbourethral glands or Cowper’s glands are paired and founded. They are situated beneath the prostate on either side of the membranous urethra. They open info the spongy urethra. They secrete a mucus-like secretion for lubrication.
![]()
Female Reproductive System
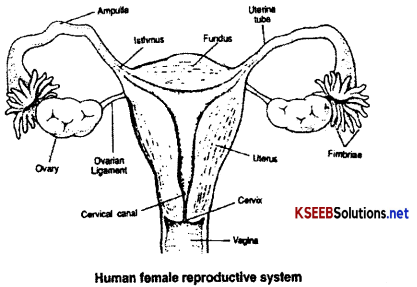
→ Female reproductive system consists of a pair of ovaries, a pair of fallopian tubes, a single uterus, a vagina, a vulva and greater and lesser vestibular glands.
→ Ovaries are paired gonads present one on each side of the uterus in the upper pelvic cavity. They are attached to the broad ligament of the uterus by a double-layered fold of peritoneum called mesovarium.-The ovaries contain a number of ovarian follicles (nearly 200,000 in each ovary at birth) in various stages of development. The ovaries produce ova, discharge them and secrete the female sex hormones, progesterone, estrogen and relaxin.
→ Fallopian tubes (uterine tubes or oviducts) are paired tubes which extend laterally it from the uterus. They transport the ova from the ovary into the uterus. Fertilization occurs in the fallopian tube. Each fallopian tube is recognised into three parts, infundibulum, ampulla and isthmus. Infundibuium is an expanded funnel shaped opening of the distal end of the fallopian tube. It lies close to the ovaiy but is not attached to it. The margin of the infundibulum is surrounded by a fringe of finger like projections called fimbriae. Ampulla is the widest and longest portion of the fallopian tube and Isthmus is the short, narrow, thick walled portion that opens into the uterus.
→ Uterus is commonly known as womb. It is a muscular, pear-shaped structure situated between the urinary bladder and the rectum in the pelvic cavity. It is the site of menstruation, implantation of fertilized ovum and development of the foetus during gestation and labour. The cavity of uterus is called uterine cavity. The uterus is divisible into an upper dome-shaped portion called fundus, a major tapering central portion called body and a narrow lower portion called cervix which opens into the vagina. The muscular axis of the uterus has three layers. The external thin membranous perimetrium, middle thick layer of smooth muscle, myometrium and inner glandular layer called endometrium.
→ Cervix secretes mucus that enhances sperm movement into the uterus and prevents the embryo from bacterial infection.
→ Vagina is a muscular canal lined with mucous membrane. It is about 10cm in length. It receives the penis during sexual intercourse and serves as the birth canal during parturition.
→ Vulva is the external genitalia which consists of mons pubis, labia majora, labia minora and clitoris. Lesser vestibular glands (Skene’s glands) are homologus to the prostate glands of the males. They are embedded in the wall of the urethra and secrete mucus. Greater vestibular glands (Bartholin’s glands) are homologus to the bulbourethral glands of the males. They are situated one on either side of the vaginal orifice. They secrete mucus which lubricates the vulva.
Hymen: The opening of the vagina is often covered by a membrane called hymen. It is often tom during the first intercourse or during active participation in some sports like horse riding, cycling etc.
![]()
Note: The presence or absence of hymen is not a reliable indicator of virginity or sexual experience.
Table showing Functions of female reproductive system
| Parts of the reproductive system | Functions |
| Ovary | Producing of ova and the female sex hormones. |
| Oviduct | Transportation of ova from the ovary to uterus. |
| Uterus | Site of menstruation, implantation of a fertlized ovum, development of the foetus and labor. |
| Cervix | Secretes mucus that enchances sperm movement into uterus and prevents the embryo from bacterial infection. |
| Vagina | Organ of sexual intercourse and birth canal |
| Lesser and greater vestibular glands | Secrete mucus that provide lubrication during sexual intercourse |
Mammary glands
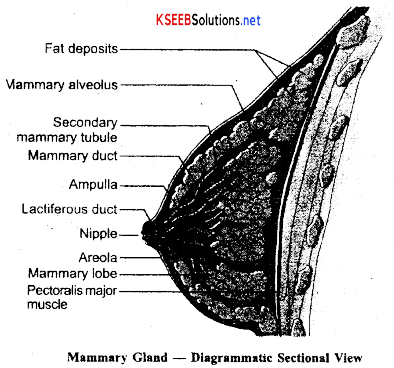
→ Human females have a pair of functional mammary glands. They are paired structures (breasts) that contain glandular tissue and variable amount of fat. The glandular tissue is divided into 15-20 mammary lobes, each lobe contains clusters of cells called alveoli which open into mammary tubules. The cells bf the of e^ch lobe join to form a mammary duct. Several mammary ducts join to form a wider mammary ampulla that is connected to lactiferous duct, through which milk comes Out.
→ Surrounding the nipple is a circular disk-like rough pigmented skin called the areola. The areola contains modified sebaceous glands to provide lubrication for the nipple during nursing.
![]()
Gametogenesis:
Production of gametes by gonads is called gametogenesis. It is of two types.
- Spermatogenesis and
- Oogenesis.
Spermatogenesis:
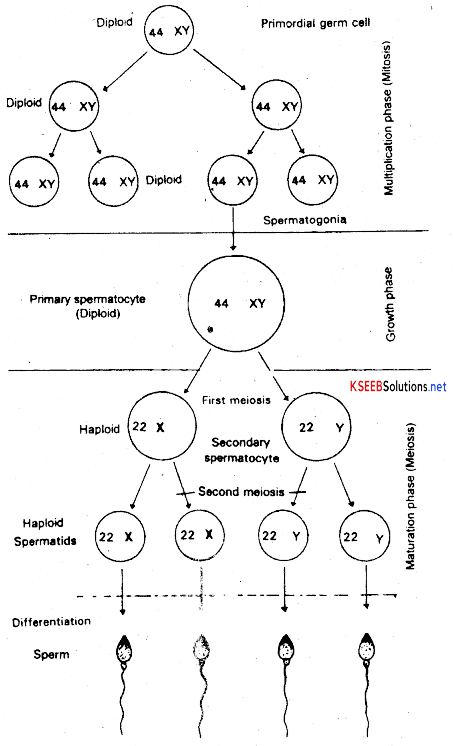
Formation of haploid sperms from the diploid spermatogonial cells of the testes is called spermatogenesis. Primordial germ cells give rise to spermatogonial cells and sertoli cells. It is the spermatogonial cells that develop into the spermatozoa. Spermatogenesis involves four phases., viz..
a. Multiplication Phase
b. Growth Phase
c. Maturation Phase
d. Spermiogenesis
(a) Multiplication Phase: The diploid spermatogonial cells of the seminiferous tubules divide repeatedly by mitosis to form more spermatogonial cells. Among them only a few will enter into growth phase and others are kept in reserve.
(b) Growth Phase: Spermatogonial cells obtained from multiplication phase grow in size, however they still remain diploid. These cells are now called primary spermatocytes.
(c) Maturation Phase: This phase involves two successive divisions, viz., Meiosis 1 and Meiosis II. The meiosis I is reductional and two haploid cells are formed from each primaiy spermatocyte. The resultant cells of I meiotic division are called secondary spermatocytes. These secondary spermatocytes undergo meiosis II which is equational. As a result each secondary spermatocyte produces two haploid cells of equal size called spermatids. Hence, four haploid spermatids are formed during maturation phase from each diploid primary spermatocyte.
(d) Spermiogenesis: Spfermatids are not gametes, they are ordinary haploid cells. During spermiogenesis or spermateliosis each spermatid in association with sertoli cells become tadpole like, flagellated and highly motile gamete called spermatozoan or sperm.
![]()
Hormonal Control of Spermatogenesis:
- Spermatogenesis is initiated due to an increase in the secretion of gonadotropin-releasing hormone (GnRH) by the hypothalamus at the age of puberty.
- The increased levels of GnRH act on the anterior pituitaiy and stimulate the secretion of two gonadotropins, i.e., luteinizing hormone (LH) and follicle stimulating hormone (FSH).
- LH acts on the Leydig cells and stimulates them to secrete testosterone.
- FSH acts on the Sertoli cells and stimulates secretion of some factors, which help in spermiogenesis.
Oogenesis:
The formation of ova or eggs from the diplod oogonial cells of the ovaiy is called oogenesis. Primordial germ cells give rise to oogonial cells, and follicular cells (nurse cells). It is the oogonial cells that develop into ova. Oogpnesis involves three phases, viz.,
- Multiplication phase
- Growth phase
- Maturation phase
1. Multiplication phase: The diploid oogonial cells of the ovarian follicles divide repeatedly by mitosis to produce more oogonial cells. Among them only a few will enter into growth phase and others are kept in reserve.
2. Growth phase: During this phase few oogonial cells synthesise yolk or vitelline in the cytoplasm and transform into primary oocytes. Hence this phase is also called vitellogenesis. During the growth of oogonial cells into primary oocytes, follicular cells or nurse cells or granulosa cells assist vitellogenesis.
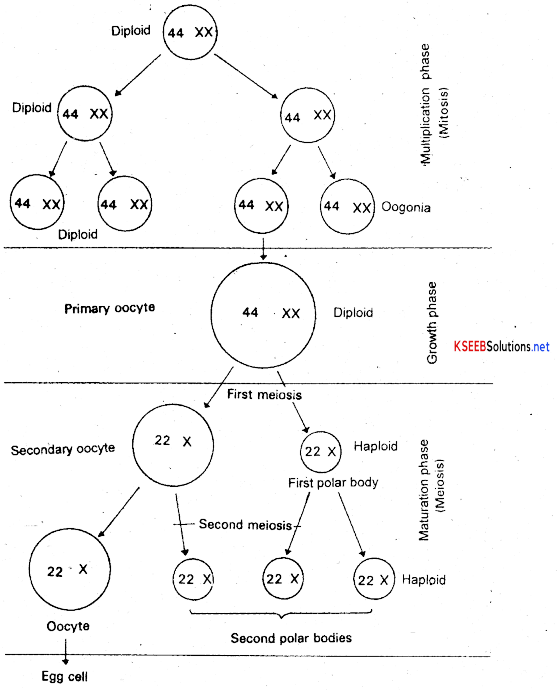
3. Maturation phase: This phase involves two successive divisions namely meiosis I and meiosis II. The meiosis I is a reductional cell division resulting in the formation of a smaller cell often called the first polar body and larger secondary oocyte. The larger secondary oocyte undergoes meiosis II to form a larger cell called ootid or ovum and a smaller cell called as second polar body. The first polar body may also undergo meiosis II to produce two more secondary polar bodies. So at the end of oogenesis one ovum and three polar bodies are formed. These polar bodies will not survive. They undergo disintegration.
![]()
Hormonal Control of Oogenesis:
- Oogenesis is initiated due to an increase in the secretion of gonadotropin-releasing hormone (GnRH) by the hypothalamus at the age of puberty.
- The increased levels of GnRH act on the anterior pituitary and stimulate the secretion of two gonadotropins, i.e., luteinizing hormone (LH) and follicle stimulating hormone (FSH).
- FSH induces the development of ovarian follicle which produces estrogen. Estrogen causes proliferation of endometrium as well as inhibition of FSH production. Increased estrogen level in the mid cycle triggers the anterior pituitary to release LH, which is responsible for ovulation as well as formation of corpus luteum.
- Corpus luteum secretes estrogen and progesterone which maintains the endometrium.
Typical structure of a sperm: Sperm is a male gamete produced m the testes by spermatogenesis. The shape and the size of the sperm varies from species to species. However all the animal sperms show a common structure.
Typical structure of sperm shows four regions. They are
a. Head
b.Neck
c. Middle piece
d. Tail
a. Head: Head is the anterior segment of the sperm which is oval in shape. Head includes a haploid sperm nucleus and a little cytoplasm. The sperm nucleus and a little cytoplasm. The sperm is devoid of yolk. The head is covered by a cap like structure called acrosome, containing hydrolytic enzymes. Acrosome helps the sperm to penetrate ovum. Acrosome is formed by golgi apparatus.
b. Neck: It is an indistinct part that connects the head and the middle piece. It includes a proximal centriole close to the sperm nucleus.
c. Middle piece: It contains a distal centriole and an axial filament. Surrounding the axial filament mitochondrial sheath (Nebenkem) is present which provides energy needed for the movement of the sperm. Hence middle piece may also be referred to as engine room of the sperm. Axial filament is also called axoneme and arises from the distal centriole which forms the axis of the tail.
d. Tail: It is divided into two parts namely,
- Main piece: It is covered by a cytoplasmic sheath.
- End piece: It is naked and forms the terminal part of the tail.
The tail shows lateral undulating motion and bring about the propulsion of the sperm.
![]()
Structure of Ovum or Egg:
Egg is a female gamete produced in the ovary by oogenesis. The size and shape of the egg vary from species to species. Following is the typical structure of an egg.
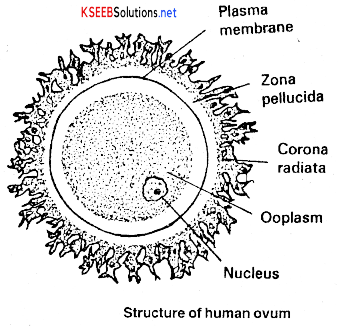
The egg is spherical or oval in shape surrounded by a plasma membrane referred to as oolemma. Outside the plasma membrane or oolemma lies another membrane called vitelline membrane. The oolemma encloses egg cytoplasm which is referred to as ooplasm and a haploid egg nucleus.
Usually, in a typical egg, the upper pole is called animal pole and the lower pole is called vegetal pole. Ooplasm towards animal pole contains colour pigments and forms animal hemisphere, whereas towards vegetal pole ooplasm contains reserve food material in the form of yolk and forms vegetal hemisphere.
Egg cytoplasm or ooplasm containing yolk is referred to as deutoplasm. The amount and distribution of yolk varies from species to species. The peripheral ooplasm is referred to as cortex of the egg and it contains cortical granules. They play a significant role in fertilization.
Menstruation:
It is a normal female periodic cycle of discharge of blood due to rupturing of endometrium of uterus. The period of menstruous cycle is about 28 days. The menstruous cycle may be divided into four phases.
1. Menstrual Phase: It is also called menses. It is a normal female periodic cycle of discharge of blood due to rupturing of endometrium of uterus. Also unfertilised egg and ruptured tissue of endometrium is discharged. It lasts for about five days of the cycle.
2. Pre ovulatory Phase / Follicular phase (Proliferative phase): Here regeneration and thickening of endometrium of the uterus occurs. Also this phase is characterized by the transformation of primary follicle into mature Graafian follicle under the influence of FSH. The secretion of gonadotropins (LH and FSH) increases gradually during the follicular phase. It takes about 6 to 13 day in a 28 day cycle.
3. Ovulation / Luteal phase (Secretory phase): During this process ovum is released from ovary in the pelvic cavity and the process is called ovulation. It occurs approximately on 14th day of menstrual cycle. It is a phase in which both LH and FSH are at the peak level and there is an LH surge.
4. Post Ovulation Phase: It is also known as luteal phase. It lasts from 15th to 28 in a menstrual cycle. After ovulation. LH stimulates the development of corpus luteum which starts secreting progesterone prepares the endometrium of the uterus to receive the fertilized ovum. However, if fertilization does not occur the corpus luteum degenerates and becomes the corpus albicans.
Note: Menarche: The first menstruation begins at puberty and is called menarche. It starts at puberty between the age of 12 to 15 years.
Menopause: In human beings, menstrual cycles ceases around 50 years of age; that is termed as menopause Menopause results due to the decline in the production of estrogen and progesterone from the ovary.
![]()
Fertilization:
→ The process of fusion of haploid spermatozoan and an haploid ovum forming a diploid zygote is called fertilization.
→ The sperms are produced in the testis and pass down into the epididymis, vas deferens and the ejaculatory duct. Ova produced in the ovaries is discharged into the body cavity. They, enter the fallopian tube and pass through the uterus and vaginal canal. The oocyte remains fertile only for about 24 hours.
→ Generally fertilization occurs in the upper part of fallopian tube. During fertilization, several sperms surround the egg. They release 3 types of lytic enzymes to disperse the cells of cumulus oophorus, to dissolve the substance holding the corona cells and to penetrate zonapellucida though several sperms surround the egg only one sperm will become successful in penetrating and fertilizing the egg.
→ The process of acquiring the capacity to fertilize the egg by sperm is called capacitation. After sperm penetration cortical granules of the ooplasm are released into the space between zone pellucida and plasma membrane, it prevents polyspermy
Early development:
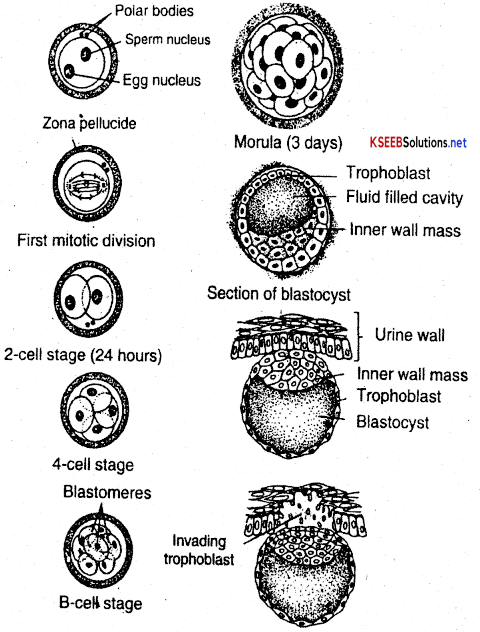
- About 24 or 36 hours after fertilization zygote undergoes holoblastic and equal cleavage.
- Asa result of successive cleavage the solid mass of cells formed called morula which is about the same size as zygote.
Formation of Blastocyst: As morula under goes further divisions it continues to move to reach the uterus within 7 days from the day of ovulation or 21st day of menstruation. Hollow spherical blastula is formed called blastocyst from morula. The outer most wall layer of blastocyst is called Trophectoderm and a layer of cells lining the blastocoel is called blastoderm. The inner fluid filled cavity called the blastocoel.
Implantation or cnidation:
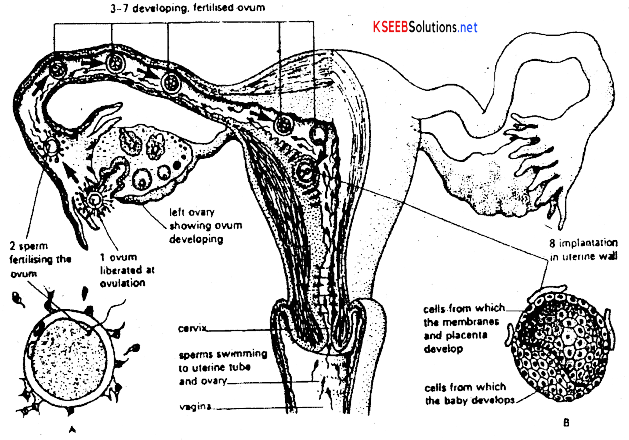
The blastocyst remains in the uterine cavity for about 2 or 3 days and then attaches itself to the uterine wall and gradually invades into it. This phenomenon of embedding of the blastocyst into the endometrium is called implanation or cnidation. It occurs either on 21st day of menstrual cycle or 7 days after ovulation.
![]()
Formation of Foetal membranes:
- Embryo develops four types of foetal membranes i.e, amnion, yolk, allantois and chorion
- Yolk sac is non functional part of umbilical cord.
- Allentois is in the form of small vascularised membrane which becomes a functional part of umbical cord.
- Amnion is in the form of a thin protective membrane which surrounds the embryo, Amniotic cavity filled with amniotic fluid which provides aqueous medium for development and serves as a shock absorber for the foetus.
- Chorion becomes a part of placenta.
![]()
Placenta:
Placenta is an organic connection between the developing foetus and uterine wall of mother for the purposes of physiological exchange. Placenta develops partly from the tissues of embryo (Trophoblast) and partly from the uterine wall of the mother. The whole structure is in the form of a flat – cake or large disc. Therefore it is called metadiscoidaltype. The embryo is attached to this disc by a tube called umbilical cord.
The foetal part of placenta is produced into a number of finger like villi called chorionic villi which penetrate into the uterine wall. The foetal blood capillaries extend into P the villi to take the foetal blood close to the blood supply of the mother in the uterine wall. The chorionic villi actually bathe in the uterine blood of the mother. Hence the placenta is called hemochorial.
In this system of arrangement the blood of the foetus and the blood of the mother are brought so close that they are separated by only the capillary walls and the membrane covering each villus. The t embryo is attached to the disc by a tube called umbilical cord. Thus there is a rope like structure found attached to the disc and other end of placenta is attached to the uterus wall.
Functions of Placenta :
- Helps in diffusion of oxygen from the maternal blood into the foetal blood.
- Helps in diffusion of carbon dioxide from the foetal blood into the maternal blood.
- Transportation of nutrients from the maternal blood into the foetal blood takes place through the placenta.
- Transportation of nitrogenous wastes from the foetal blood into the maternal blood takes place through the placenta.
- Placenta stores glycogen and acts as a liver before the formation of the liver in the foetus.
- Placenta secretes hormones like progesterone, human chorionic gonodotropin (HCG) human chorionic somatotropin (HCS) or human placental lactogen (HPL) and relaxin.
Note:
1. Umbilical cord : It is a long tube – like structure formed by the allantois and the yolk sac of the foetus. It connects tHe foetus to the disc like placenta. The umbilical cord carries an artery and a vein of the developing foetus. These blood vessels form a dense network of blood capillaries which extend throughout the disc of the placenta.
2. Pregnancy: The period of development between fertilization and birth of baby is called pregnancy or gestation. It is the sequence of events that includes Fertilization, implantation foetal growth and birth. Pregnancy lasts approximately 914 months or 280 days in human females.
Embryonic development: Simultaneous to the development of placenta, the inner cellmass differentiates into an outer layer called mesoderm, inner layer endoderm and a middle layer called mesoderm. These primary germ layers give rise to all the tissues and organs of the adult.
- After one month of pregnancy, the heart is formed.
- By the end of second month, limbs and digits develop.
- By the end of third month-organ systems are formed.
- By fifith month hair erupts on the head! Foetus also shows movements.
- By end of sixth month eyelids, eyelashes and hair are formed.
- By end of eight month testes desend into the scrotum.
- By end of nine months foetus is completely developed and ready for its delivery.
![]()
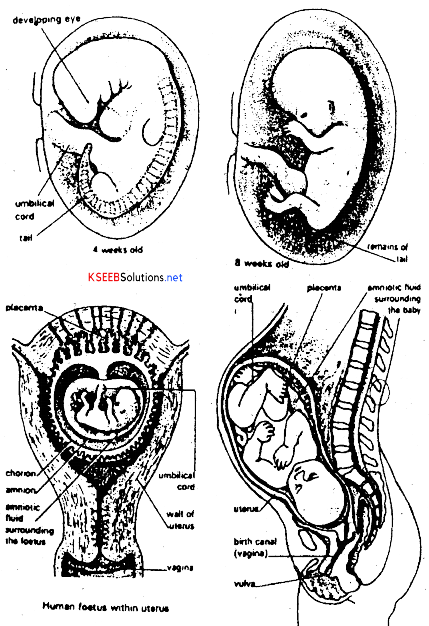
3. Parturition: It means birth, parturition is accompanied by a sequence of events referred to as labor. A few days before birth, the baby turns within the uterus until its head lies towards the cervix. This is called head fixation. The hormones oxytocin and relaxin influence powerful and frequent contractions of the urterine muscles. It results in the propelsion of the baby out of the body of the mother.
Lactation: The mammary glands also undergo certain development during pregnancy under the influence of hormones like prolactin and progesterone.
Lactation is the secretion of milk from the mammary glands.
The milk produced during initial few days of lactation is called colostrum which is yellow in colour, containing several antibodies to provide passive immunity to the new born baby.